Abstract
Musculoskeletal injuries are one of the most common types of both battlefield and civilian injuries. Early and reliable stabilization is important to prevent further injury, minimize pain, and facilitate transport for follow on treatment.  Splints and plaster casts are the most common methods for stabilizing a fractured limb; however, these methods can take considerable time and resources to implement, and improper application can cause serious complications including ulcers and compartment syndrome. As part of our research, we interviewed doctors, first responders and reviewed the literature (e.g. AO Manual of Fracture Management), and found that many of the challenges with limb stabilization can be addressed with concepts from soft material robotics. This work presents a patent pending advanced splint that is portable, modular, quick to apply (< 1 min.), easy to remove, safely conforms to a limb, and can accommodate limb swelling.
ProblemÂ
An important step in treating any fracture is to stabilize the limb to prevent the fracture site from causing vascular damage until the patient can receive definitive care. Traditional methods for stabilizing a fractured limb include splints, which are typically used in austere environments, and plaster casts, which are typically applied in the hospital.
These methods are effective at stabilizing the limb; however, improper application and/or poor monitoring can cause serious problems. For example, splints can cause pressure points, which over a matter of hours can turn into ulcers and necrotic tissue. Alternatively, swelling of the fracture site combined with tight bandages under splints or casts can increase the risk for compartment syndrome, which can lead to amputation if not monitored carefully.
Furthermore, the application methods employed to avoid these downstream complications slow the stabilization treatment process. This can be problematic in multiple casualty scenarios where the time spent stabilizing one patient is time that could be spent treating another.
Solution
The functional requirements that guided the design of the advanced splint included
- provide 1st order alignment (i.e. make the leg look like a leg)
- provide open wound access
- accommodate a range of limb sizes
- portability
- quick to deploy
- compatible with existing standard of care
- easy to remove
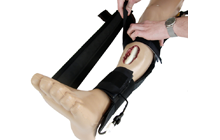
The video above presents a splint that unfolds from a small pack to a structure that can stabilize an entire leg. Inflatable collars act as anchor points along the leg with integrated check valves to prevent over pressurization. The collars are connected to a patent pending rigidizing beam that provides 1st order alignment with only 8 psi. Furthermore, the collars are designed to slide along the beam to accommodate a range of tip-fib sizes and wound locations. The splint can be activated from a single inflation source, and applied in less than 1 minute (note: non-pneumatic stabilization solutions were patented as well).